에스트로겐 개요 및 선택 가이드
Estradiol (E2) is the core medication in transgender women’s HRT. When selecting a route of administration, safety (specifically the risk of Venous Thromboembolism, or VTE) should be your primary consideration, rather than just convenience or cost.
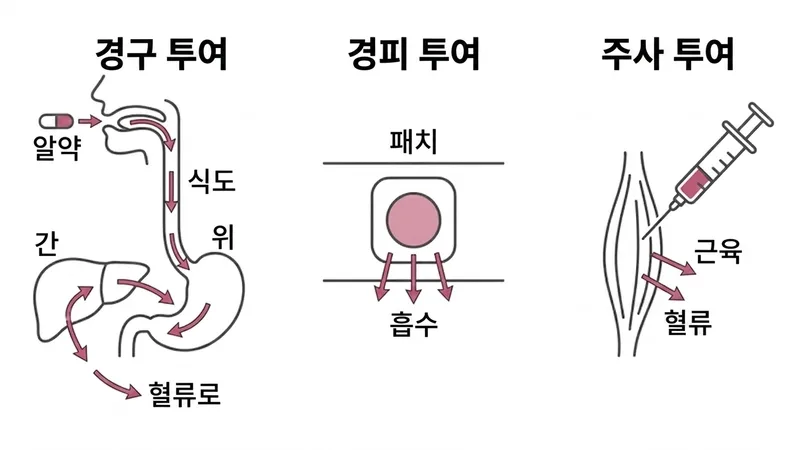
VTE Risks by Administration Route
섹션 제목: “VTE Risks by Administration Route”Venous Thromboembolism (blood clots) is one of the most severe risks associated with estrogen therapy. The risk varies dramatically depending on how the estrogen enters your body [1] .
| Route | Relative Risk (RR) | Evidence Level | Note |
|---|---|---|---|
| Transdermal Patch | RR ≈ 0.97 | A | No significant risk increase vs. non-users |
| Transdermal Gel | RR ≈ 0.97 | A | Similar to patches, bypasses liver first-pass |
| Oral (Estradiol Valerate/Hemihydrate) | RR ≈ 1.48 | A | Risk increased by ~48% |
| Sublingual | Limited Data | C | Partially bypasses first-pass, theoretically lower than oral |
| Injectable (EV/EC/EEn) | Limited Data | C | Bypasses first-pass, but lacks large RCT data on clot risks |
Route Selection Guide
섹션 제목: “Route Selection Guide”The following framework is built upon current clinical evidence [2] [3] :
Scenario 1: Existing VTE Risk Factors
섹션 제목: “Scenario 1: Existing VTE Risk Factors”Risk Factors include: Age >40, BMI >30, smoking, family history of VTE, history of clotting disorders, or migraines with aura.
- Preferred: Transdermal Patch or Transdermal Gel
- Avoid: Oral Estradiol
- Also Avoid: Combining oral estrogen with Cyproterone Acetate (CPA)
Scenario 2: No VTE Risk Factors
섹션 제목: “Scenario 2: No VTE Risk Factors”Choose based on accessibility, budget, and personal preference:
- Oral Estradiol (Estrace, Progynova): Generally the most affordable and widely accessible route globally.
- Transdermal Patch (Climara, Estradot): Superior safety profile, but can be expensive or suffer from global supply chain shortages.
- Sublingual: Uses oral pills dissolved under the tongue. Higher bioavailability but creates massive spikes/drops in blood levels.
- Injectables: Causes significant peak/trough fluctuations but is highly effective for monotherapy.
Scenario 3: Monotherapy (Estrogen Without Anti-Androgens)
섹션 제목: “Scenario 3: Monotherapy (Estrogen Without Anti-Androgens)”If you wish to suppress testosterone using solely estradiol without taking a dedicated anti-androgen blocker:
- Preferred: Injectable Estradiol (EV, EC, EEn) – reliably maintains the consistently high E2 levels required.
- Alternative: High-dose transdermal patches (200-400 µg/day) or transdermal gel.
- Reference: A 2025 study by Misakian demonstrated that 82.6% of users on an injectable EV monotherapy regimen achieved T suppression without needing an anti-androgen [4] .
Pros & Cons Quick Reference
섹션 제목: “Pros & Cons Quick Reference”| Route | Pros | Cons | Typical Accessibility |
|---|---|---|---|
| Transdermal Patch | Lowest VTE risk; stable blood levels; change 1-2 times weekly | Skin irritation; can be expensive or frequently out of stock globally | Moderate |
| Transdermal Gel | Low VTE risk; flexible daily dosing | Absorption varies wildly by skin type; requires drying time | Moderate |
| Oral (Pills) | Easiest to access; very cheap; simple to take | Higher VTE risk; liver first-pass metabolism wastes a lot of the drug | Very High |
| Sublingual | Higher bioavailability than oral; partially bypasses liver | Massive spikes and dips in blood levels; requires dosing 2-3 times daily | Very High (Uses oral pills) |
| Injectable (EV/EEn) | Bypasses liver; highly effective for monotherapy | Requires needles/injection anxiety; intense blood level peaks and troughs | Varies by country (often DIY) |
Dosage Overview
섹션 제목: “Dosage Overview”Standard dosage ranges across different routes [2] [3] :
| Route | Starting Dose | Maintenance Dose | Typical Max Dose |
|---|---|---|---|
| Transdermal Patch | 50-100 µg/day | 100-200 µg/day | 400 µg/day |
| Transdermal Gel | 1.5 mg/day | 3 mg/day | 6 mg/day |
| Oral Estradiol | 2 mg/day | 4 mg/day | 8 mg/day |
| Sublingual | 1-2 mg/day (split 2-3x) | 2-4 mg/day (split 2-3x) | 6 mg/day |
| Injectable EV | 1-2 mg/week | 2-4 mg/week | 5 mg/week |
Detailed Pages
섹션 제목: “Detailed Pages”For deep dives into the pharmacology, usage methods, and specific warnings for each route, click below:
- Transdermal Patches — The safest administration route
- Oral Estradiol — Highly accessible but carries slightly elevated VTE risks
- Sublingual — A compromise offering higher absorption but dramatic fluctuations
- Transdermal Gel — Flexible safety that sits between patches and oral
- Injectable Estradiol — The gold standard for monotherapy